General Information
Thank you for choosing to deliver your baby at Scarborough Health Network (SHN). We look forward to providing you with an outstanding care and delivery experience.
Our Birthing Centres are nationally recognized for providing culturally sensitive, respectful, and responsive care that meets our patients’ unique needs.
Our Neonatal Intensive Care Units (NICUs) are located at our Centenary and General hospitals, and are able to look after newborns as premature as 30 gestation.

Take a tour of our Family Birthing Centres
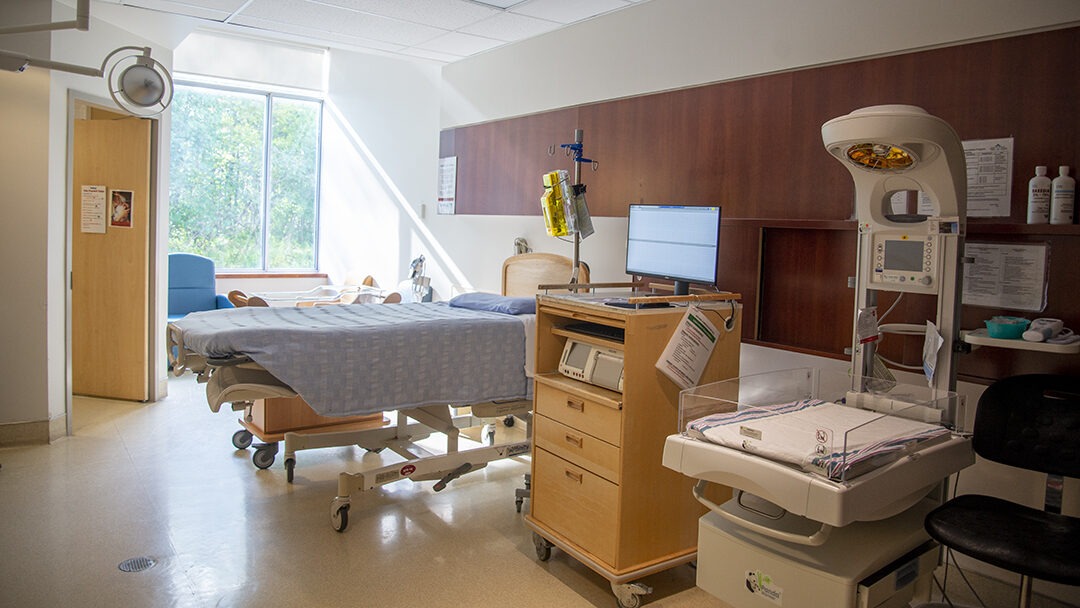
Let us show you around! Whether you have already registered to have your baby at Scarborough Health Network or you just want to learn more about us, we are excited to welcome you to our Family Birthing Centres at both Centenary Hospital and General Hospital.
We invite you to book a tour with us, or browse through some of our photos.






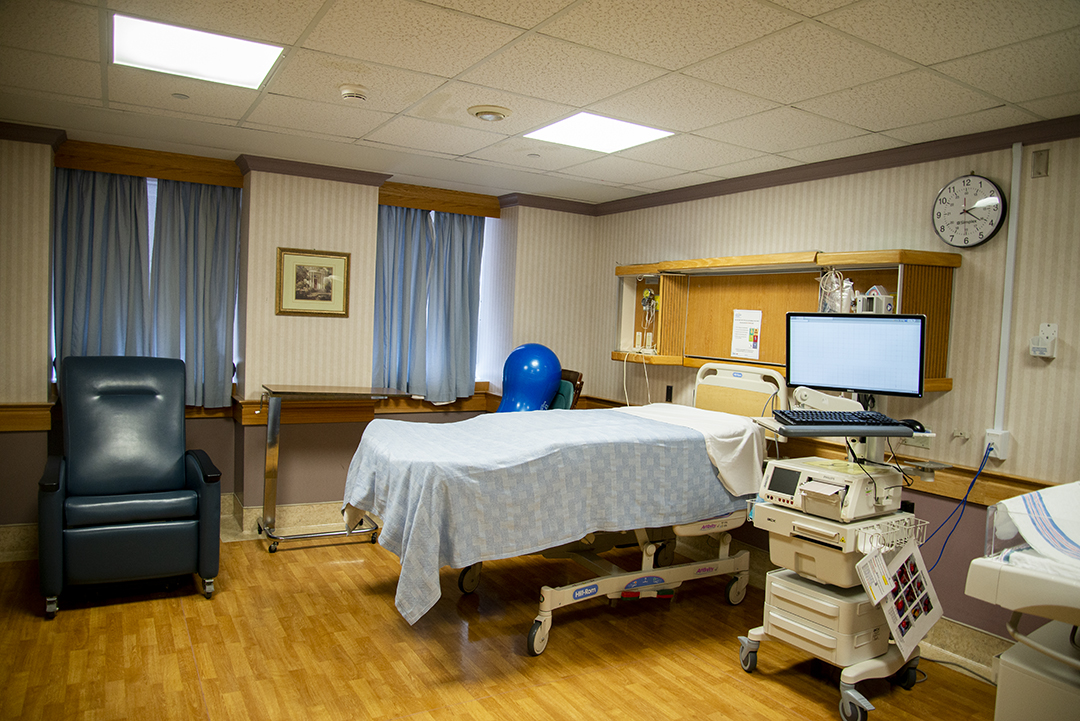

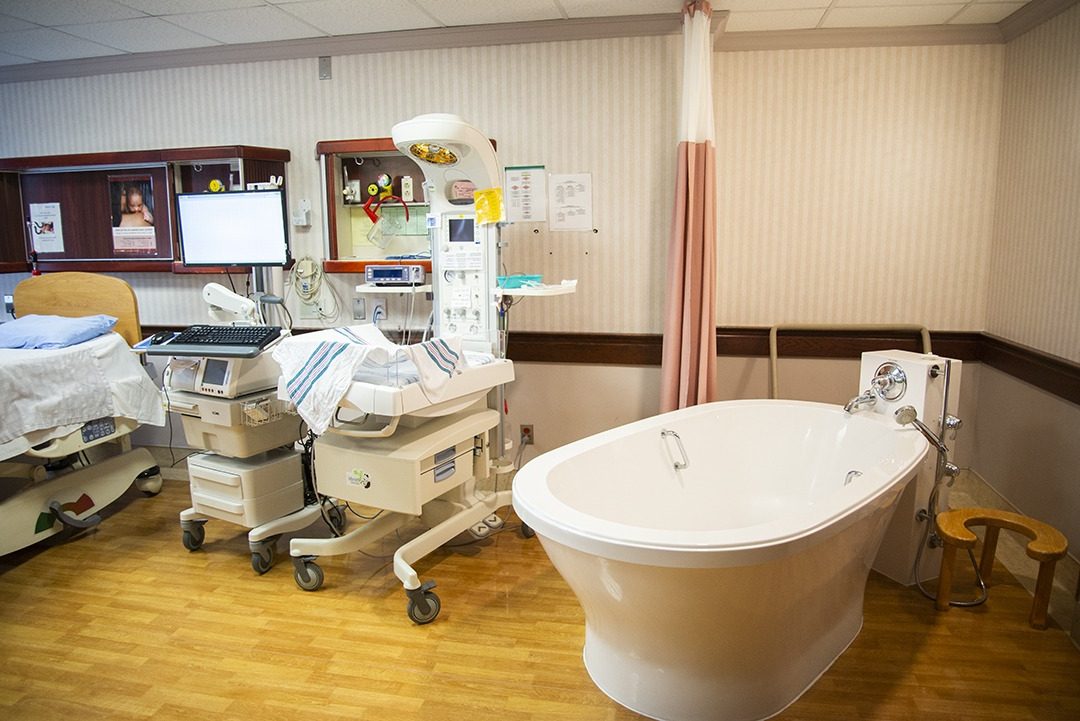
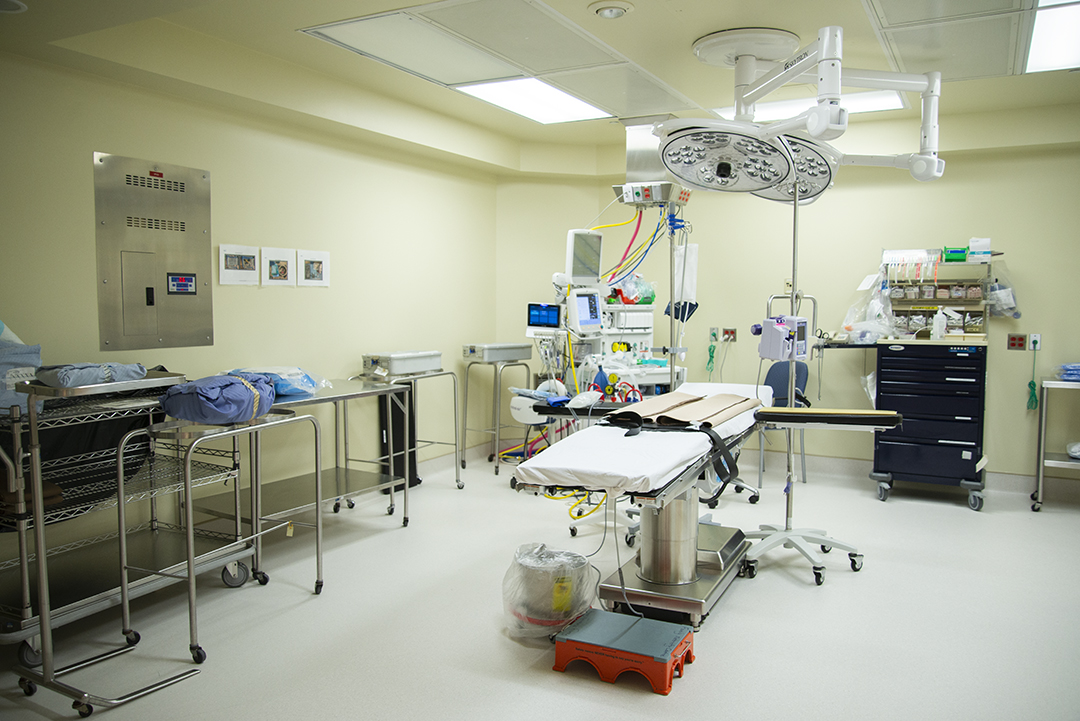
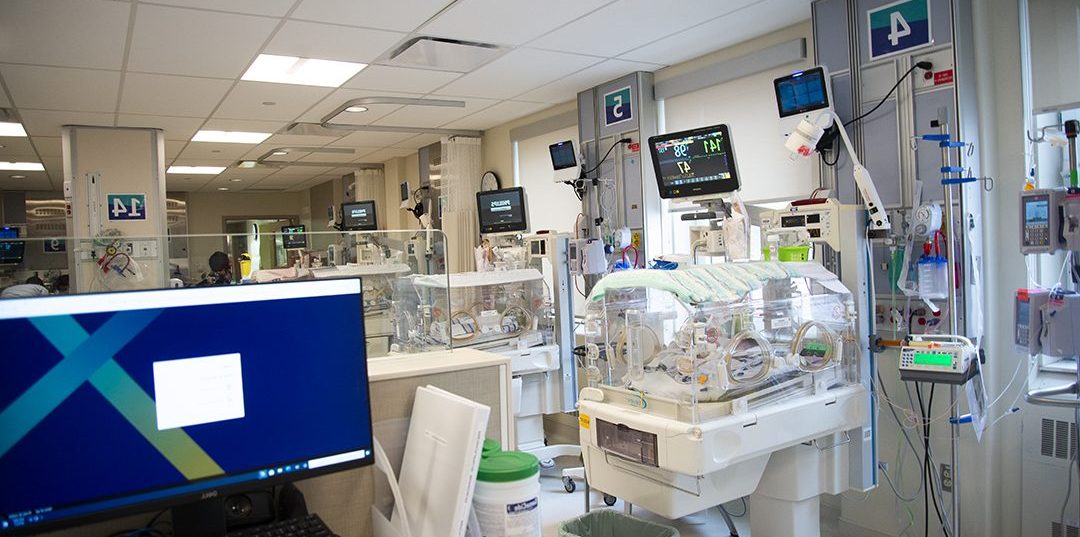
Getting Care During Your Pregnancy
Pregnant individuals who receive early and regular prenatal care generally have better outcomes. Getting care during your pregnancy is essential for both the birth parent and baby’s health. At SHN, we offer multitudes of services and resources to make expecting families’ journeys safe, inclusive and accessible.

Planning Your Pregnancy
Even the most healthy pregnant individuals can have pregnancy problems but taking steps towards a healthy lifestyle can increase your chances of having a healthy pregnancy. We offer advise and education for expecting families on how to maintain a healthy lifestyle, providing better outcomes.
Folic Acid
The best way to reduce the risk of your baby developing a neural tube defect is to take daily folic acid supplements from 12 weeks before conception until at least 12 weeks of pregnancy. Folic acid is very important because it can help prevent some major birth defects of the baby’s brain (anencephaly) and spine (spina bifida).
Preconception care involves any intervention that can identify and modify medical, psychosocial, behavioural or environmental risks to female or male reproductive health and future pregnancies.
At SHN, we are able to assess the risk and outcomes of future pregnancies for people who have had previous complications in pregnancy or who have complicated medical conditions. In addition, our clinic offers counselling to people about choices for prenatal diagnosis of multiple chromosomal and genetic disorders. We also assess future or current pregnancy complications in people with a history of genetic disorders.
Our Pregnancy Care Providers
Deciding who to choose for your pregnancy care and childbirth is an important decision. The information below may help you decide.
Our obstetricians work with pregnant people and families to keep pregnancies healthy and to deliver babies. In addition, your OBGYN may address general health needs, such as screening for other health issues, prescriptions and other issues.
We have some of the best obstetricians to look after your pregnancy and deliver your baby. If you would like to see one of our obstetricians for your prenatal care, please have your family doctor make a referral.
Midwives provide care throughout women’s pregnancy, labour, and birth, as well as care for moms and their newborns six weeks after birth. At SHN, midwives are part of our team. We have partnerships with three midwifery organizations. For more information, or to make an appointment, please contact them.
Diversity Midwives
416-609-8187
info@diversitymidwives.com
Sages-Femmes Midwives
416-286-2228 or 905-409-6447
rougevalleymins@gmail.com
Trillium Midwives
905-668-8520
info@trilliummidwives.ca
Ontario midwives are funded by the Ontario Ministry of Health and Long-Term Care and services are free to clients.
Our patient and family centered environment supports the education of our learners and the evaluation and research of our practices and outcomes. Our maternity care team includes physicians, family medicine residents, nurses, a dietitian, pharmacist and nurse practitioners and supports patients through all phases of pregnancy, birth and postpartum care.
Our Clinics and Services
The Early Pregnancy Assessment Clinic (EPAC) at SHN provides prompt assessment of pregnant individuals who are less than 20 weeks and are experiencing complications of pregnancy. Patients will be seen by a registered nurse and obstetrician.
Services provided
The clinic provides access to ultrasound, blood testing and surgical interventions as needed and indicated. Referrals to SHN’s genetic clinic, homecare and other services can be facilitated through the clinic if necessary.
How to Access Care
Clinic Hours
Monday, Wednesday, Friday 7:30 a.m. – 2:30 p.m.
Clinic Location
SHN General hospital, 3050 Lawrence Avenue East
2nd floor, Family Maternity Centre (FMC)
- Register before your appointment at a Registration Kiosk on the ground floor
- Your health card is required at each visit
- Take the East Tower (Green) Elevators to the 2nd floor
- Check in for your visit directly with the EPAC nurse. The clinic is located beside the fish tank.
Contact
Phone: 416-431-8143
Fax: 647-598-4004
Ocean e-Referral
We are now accepting Ocean eReferrals! For additional information, please email your Ontario Health East Deployment Team at contact@ereferralontarioeast.ca
SHN, the Scarborough Ontario Health Team (SOHT), and Scarborough Family Physicians Network (SFPN) are working together to support healthcare providers in our community who may be interested in onboarding onto Ocean. Get started by completing the Ontario Health East online form.
If your pregnancy needs close monitoring because you’re having twins, or have high blood pressure or diabetes, your doctor or midwife can refer you to this clinic for ultrasound testing and other non-stress tests and services.
For pregnant individuals with higher risk pregnancies due to medical issues, including hypertensive disorders, gastrointestinal disorders, respiratory disease, hematological conditions, and rheumatological conditions.
This clinic offers consultation with an Internist or pregnant individuals with higher risk pregnancies due to medical issues, including:
- Hypertensive disorders
- Gastrointestinal disorders
- Respiratory disease
- Hematological conditions
- Rheumatological conditions
This clinic offers consultation with an Internist.
Contact Us
Call for appointment inquiries: 416-431-8167
Fax referral forms: 416-495-2581
The Maternal Fetal Medicine (MFM) Clinic is for higher risk pregnancies such as:
- Complicated twin gestations
- Pregnancies with anatomic or placental concerns
- Pregnant individuals with maternal or parental medical conditions affecting pregnancy
Preconception consults for medical conditions or obstetric history are also welcome. This clinic offers consultation with an MFM specialist and specialized ultrasound assessment.
Contact us
Call for appointment inquiries: 416-431-8167
Fax referral forms: 416-281-7102
If you are pregnant and have diabetes or develop diabetes in your pregnancy the diabetes education clinic will help to guide you and provide information concerning diet, activity and how to safely monitor your blood glucose levels. Interdisciplinary team (dietician, nurse, endocrinologist).
The Genetics clinic at SHN is located at our Centenary hospital. Through this clinic, we offer genetic counseling services to expectant couples. Some of the indications we offer consults for are:
- Couples at an increased risk to have a baby born with a known genetic condition (such as sickle cell disease or thalassemia)
- Couples with an abnormal ultrasound findings
- Couples with a high-risk screening result (through Non Invasive Prenatal Test, or First Trimester Screen with a risk greater than 1 in 20)
- Couples with a personal and/or family history of a genetic condition or a chromosome abnormality
- Newborns with a congenital anomaly, or a known or suspected genetic condition
Services
Our team consists of genetic counsellors and a physician geneticist. Genetic procedures and testing can be arranged at various hospitals and laboratories, as appropriate.
Contact information
Call for appointment inquiries: 416-431-8167
Fax referral forms: 416-495-2581
A referral from your midwife or doctor will be required.
Ocean eReferral
This clinic now accepts Ocean eReferrals! For additional information, please email your Ontario Health East Deployment Team at contact@ereferralontarioeast.ca.
Registering for Ocean
SHN, the Scarborough Ontario Health Team (SOHT), and Scarborough Family Physicians Network (SFPN) are working together to support healthcare providers in our community who may be interested in onboarding onto Ocean. Get started by completing the Ontario Health East online form.
Prenatal breast/chest feeding classes are offered to expectant families. The classes are led by lactation consultants, who teach about:
- What to expect in the first few days after your baby is born
- The benefits of breast/chest feeding
- How to breast/chest feed and be confident in your ability
- What is a good latch
- How often to breast/chest feed and how to know if baby is getting enough
- Breast/chest feeding myths and facts, common challenges and solutions
- Hand expressing, breast pump options, and how best to store expressed breast milk
- Breast/chest feeding supports available at Scarborough Health Network and within the community
Classes at Centenary Hospital
One-hour sessions are offered twice a month from 2 – 3 p.m. on weekends. No registration is required.
For more information call 416-284-8131 ext. 4530
Classes at General Hospital
Classes are held every fourth Wednesday of the month from 1 – 2:30 p.m. in the Global Community Resource Centre, ground floor. Registration is not required.
For more information call 416-438-2911 ext. 83222
Prenatal Classes
Prenatal and childbirth education classes provide families with important information and skills preparation that are fundamental to childbirth and the first few weeks of parenthood. Our prenatal classes are taught by qualified labour and delivery nurses who will guide you through everything that you need to know about having a baby – from what to do when you go into labour, to important tips for caring for your newborn. Each class is about eight hours, from 9 a.m. to 5 p.m.
Having Your Baby at SHN
Pregnancy is a very special time. Through a number of resources, we can support you during your exciting journey. At SHN, we support childbirth as a natural process. It is our goal to ensure you have a safe, inclusive and meaningful experience that respects your personal, cultural and spiritual choices.

Coming to the Hospital
Labour consists of four stages, including recovery. On average, labour for first time pregnant individuals can take up to 14 hours and those who’ve undergone childbirth before can expect about seven hours of labour.
Some of the signs and symptoms of going into labour may include:
- Period-like cramps
- Backache
- Contractions
- Your water has broken
What to Bring to the Hospital Checklist
We encourage you to bring only what you will really need while you are in the hospital. Please leave valuables at home. The following labour and delivery checklist is a guide for the important items you may need.
For the expecting persons
- Your health card
- List of current medications (including vitamins and herbal supplements)
- Your birth plan and pre-natal medical records, if you have a midwife
- Robe, dressing gown, wrap, sweater
- Slippers and/or socks
- Lots of undergarments
- An old nightdress or a t-shirt to wear while in labour
- Massage oil or lotion, if needed
- Snacks and drinks
- Things to help you relax or pass the time, such as books, magazines, games, etc.
- A headband or hair elastics
- Pillows
- Personal toiletries, such as shampoo, soap, toothbrush, toothpaste, lip balm, and tissues
- Music and player
For the birth partner/support person
- Comfortable shoes
- A change of clothes
- Watch with a second hand to time contractions
- Your choice of recording device (mobile phone or a camera)
- Address book or a list of phone numbers
- Snacks and drinks
For the expecting person
- Comfortable outfits
- Nursing bras (2-3)
- Breast/chest pads
- Nursing pillow
- Feminine hygiene products (about 20 liners)
- Nightshirt wrap or t-shirt suitable for breastfeeding
For your baby
- An infant car seat (be sure to check the expiry date)
- Two or three sleepers for baby to wear while in hospital
- Baby blankets
- Burp cloths or receiving blankets
- Diapers, baby wipes, and baby blankets
- Socks
- Hats
- One outfit for the trip home (all-in-one stretchy outfits are easiest)
- Pen to complete hospital documents
Arriving at the Birthing Centre
You are encouraged to call and speak to the nurse before coming to the Birthing Centre triage.
Centenary Hospital
416-284-8131 ext. 4047
General Hospital
416-431-8146
When you arrive at the Birthing Centre, you will be immediately assessed in our triage room to determine if you are in labour and a decision will be made as to whether or not you should stay or go home.
An experienced obstetrical nurse will perform the initial assessment and answer your questions and concerns. The on-call obstetrician will also assess you and determine if you are in labour and should be admitted to the hospital. We have obstetricians available 24/7.
The nurse will ask you questions related to your pregnancy and your present condition. Your physical assessment will include your vital signs and listening to your baby’s heart rate. If needed, an internal examination may be performed.
- If you have a birth plan, please give it to the triage nurse.
- One support person may accompany you and stay with you in the triage room. Others will be asked to wait in the waiting room.
- Your questions are welcome at any time during your stay in the triage room. Please let us know if you need translation or interpretation services.
- Most women are encouraged to walk around, eat, and drink once the initial assessment has been completed.
Birthing Procedures
An induction is a way to start labour. There are many different ways for this to be done and the method is influenced by your specific situation. Examples of these are:
- Breaking your water
- Medication like intravenous (IV) oxytocin, prostaglandin gel
- Prostaglandin gel
- Dinoprostone
- Foley induction
There are many reasons why your care provider may suggest an induction, such as:
- Medical Concerns
- It has been 12 hours since your water has broken and you are not in labour
- You have broken your water and you are Group B Streptococcus (GBS) positive
- You are over 41 weeks pregnant
- Your care provider has told you your baby is at risk
In a vaginal birth, the baby will come out through the birth canal. Most pregnant individuals give birth at around 38 to 41 weeks of pregnancy. However, there is no way to know exactly when labor will happen.
Caesarean section, sometimes referred to as C-section, is the surgical delivery of a baby through incisions in the abdomen and uterus. The objective of a caesarean section is to preserve the health of the pregnant person and/or the baby when a vaginal birth is considered unsafe.
Most caesarean sections are done under spinal or epidural anaesthesia and the pregnant person is awake. The partner/support person may be present for emotional support and to see the baby during the birth. An epidural blocks the pain, but you may still feel touch and stretching.
The baby is usually born within about 10 minutes and it take about 30-40 minutes to close the incision back up again. General anaesthesia may be necessary is it is an emergency situation, if the epidural is not working adequately or cannot be used. When general anaesthesia is used, the support person is not usually permitted in the operating birthing room.
When you have had a previous caesarean section you generally have two choices on how to deliver in your next pregnancy:
- Trial of Labour after Caesarean Section (TOLAC): an attempt at a vaginal delivery. Most pregnant people have success and have a vaginal birth after caesarean (VBAC).
- Elective Repeat Caesarean Section (ERCS): a planned repeat caesarean section (CS)
Pain Relief Options
Your labour and delivery nurse or your midwife can instruct you in breathing exercises and other methods. These can all help make you more comfortable during labour. A doula may also be available to assist you. Coupled with these more natural techniques, we offer Jacuzzi tubs for natural water therapy, which some women find very relaxing.
A mixture of nitrous oxide (laughing gas) and oxygen can be provided for you to breathe. You have to start breathing the gas as soon as you feel a contraction. The gas will make the contraction more comfortable, but it will not take away the pain or harm your baby. You may feel lightheaded.
Your obstetrician can order narcotic medication to be given intravenously or into your muscle. This medication will provide some pain relief, but it won’t take all the pain away. The medication can make you drowsy and nauseous.
All of the previous methods will make you more comfortable, but you will still have some discomfort. Some women will want more pain relief, which can be provided with an epidural anaesthetic, administered by the anaesthesiologist. Epidurals can provide very good pain relief. The anaesthesiologist will speak with you first to determine if it is safe to perform an epidural anaesthetic. In some women, due to certain medical conditions, it may be unsafe to perform this procedure.
Placing an epidural
Local anaesthetic is injected in your skin on your back to numb it and a needle is then inserted through the numb area. A thin plastic tube is then inserted through the needle and the needle is removed. Medication is injected through the plastic tube and this takes away the pain. It usually takes about 20 minutes for the medication to work. The plastic tube allows medication to be given continuously to keep you comfortable as long as you are in labour. It can also be used to provide pain relief for a Caesarean section, should you need it.
Spinal anaesthetic
With a spinal anaesthetic, a small needle is inserted into your back and the sack covering your spinal cord is punctured. A small amount of anaesthetic is injected into the fluid surrounding your spinal cord and the needle is removed. Pain relief is immediate; however, it will only last for one to two hours.
Combined spinal/epidural
With this method, a spinal anaesthetic is performed first and an epidural catheter is placed through the same needle. This provides the immediate pain relief and allows for continued pain relief with the use of the epidural catheter.
Side Effects of Epidural or Spinal Anaesthesia
You blood pressure may decrease. Your nurse will monitor your blood pressure frequently so that any unsafe decrease in blood pressure can be treated. Your legs may become weak and numb. This may prevent you from walking. Your skin may feel itchy.
Complications of Spinal Epidural/Anaesthesia
Your anaesthesiologist is a highly trained physician who will safely perform this procedure; however, despite this, complications can occur. The most common complication is a headache and it happens in 1 out of 100 patients. The headache can be severe and last for several days. Your anaesthesiologist can provide treatment if you require it. Serious complications, such as seizures, death, or permanent paralysis are rare. The risk of permanent paralysis is about one out of 200,000 patients.
Additional Hospital Services and Education
If you plan to have your baby son circumcised, it should ideally be performed within four to 14 days after birth. This can help minimize bleeding and complications. However, the procedure may be performed as early as 24 hours after birth and before your baby is one month old. Please speak with us for more information.
During your stay, your baby will be tested for:
- Heart rate, temperature, breathing
- Physical exam within 24 hours
- Bath at 18 hours of age if baby sugars and temperature is stable (can also be deferred until at home)
- Blood sugar if baby is very small or very large, you have taken labetalol in your pregnancy or you have diabetes
- Hearing test (may be conducted offsite)
- Ontario Newborn Screen
- Bilirubin (to check for jaundice)
During pregnancy, blood circulates between the pregnant person and the baby through the placenta and the umbilical cord. The blood in the umbilical cord contains stem cells. Stem cells are usually found in the bone marrow and are responsible for the production of blood cells.
You have the option of storing your baby’s cord blood in case it is needed in the future. The cord blood can be used for the baby or for other family members. Many children with leukemia or other diseases have been saved through cord blood collection.
Umbilical cord blood stem cells have been used to successfully treat diseases requiring bone marrow transplantssuch as leukemia, Hodgkin’s disease and aplastic anemia.
Getting Support After Going Home
Parents who’ve delivered their baby at SHN are generally discharged 24 hours after giving birth. Pregnant persons who’ve undergone a c-section will be required to stay at least two to three days to ensure there is no complications.
We offer a number of resources and information that will support families after they’ve left the hospital and begin their new journey.
It’s important to note: a car seat is required by law when leaving the hospital. Please ensure you have one ready for discharge.

Our Services
The Newborn Assessment Clinic offers a wide range of services for patients and babies after they are discharged from the Birthing Centre or Neonatal Intensive Care Unit (NICU).
The Neonatal Follow-Up Program (NFUP) is a multidisciplinary screening clinic that works with families to focus on their child’s development by identifying any areas of concern, teaching parents activities that can support their baby, and/or referring their child to community agencies for ongoing guidance through treatment and consultation.
Our Services
The NFUP clinic has a Paediatric Neurologist, Occupational Therapists, and Speech-Language Pathologist. The clinic monitors infants who are born prematurely with a birthweight below 2000 grams, who are small for gestational age (<3rd percentile), and/or born at a gestational age that is less than 33 weeks plus 6 days. Infants who are born with significant medical concerns may also be monitored. Infants are monitored between the ages of 4 and 24 months to identify any concerns with their growth and development.
At your appointment, the team assesses your baby’s motor, cognitive and speech and language development. Appointments usually take between 45-60 minutes. In order to improve the lives of these infants, it is important that families attend their appointment to ensure early identification of developmental concerns and intervention.
Contact Us
Centenary, 12th Floor Galaxy 12
Phone: 416-281-7476
Fax: 416-281-7313
Medical Mall at SHN – General Hospital
3030 Lawrence Ave. E., Suite B07
Phone: 416-438-2911 Ext. 86120
Fax: 416-292-9678
SHN provides a number of breastfeeding supports to help families make an informed decision on how to feed their baby. From providing best evidence and knowledge about breastfeeding to bedside breastfeeding guidance by trained nurses, we ensure that expecting families feel supported every step of the way.
Where to Find Us
Centenary Hospital
Main floor (2nd floor)
416-284-8131 ext. 4047
General Hospital
2nd Floor, East Wing
416-431-8138
Centenary Hospital
Main floor (2nd Floor)
416-284-8131 ext 7231
General hospital
2nd Floor
416-438-2911 ext. 83272
SHN offers comprehensive services and timely care at all three hospital emergency departments, however, please note: there is no obstetrician on site at Birchmount. Patients with obstetrics needs are asked to visit Centenary or General wherever possible. There are no Obstetrical services at the Birchmount hospital.
SHN’s Birchmount Hospital
3030 Birchmount Road
SHN’s Centenary Hospital
2867 Ellesmere Road
SHN’s General Hospital
3050 Lawrence Ave E.
Tour our Family Birthing Centres
We invite you to book a tour with us, or browse through some of our photos.


















At some point in your pregnancy, or after the birth of your baby, you, your health care provider or your nurse may feel a need for the assistance of a social worker. A social worker can help you with:
Social worker can also assist families with: